Career Intentions in Paediatric Surgery: A Cross-Sectional Study Of Junior Surgical Residents In Nigeria And Implications For Workforce Development
Main Article Content
Keywords
Paediatric surgery, Career choice, Surgical education, Surgical Workforce, Residency training, Nigeria
Abstract
Background: The global shortage of paediatric surgeons underscores the need to understand what influences young doctors to pursue this specialty. In Nigeria, paediatric surgery workforce density remains suboptimal. This study explored the proportion of junior surgical residents intending to specialize in paediatric surgery and identified factors that influence their career decisions.
Methodology: A cross-sectional study was conducted among junior surgery residents attending the West African College of Surgeons Integrated Revision Course in Clinical Surgery. Data were collected via self-administered online questionnaires and analyzed with SPSS version 20.
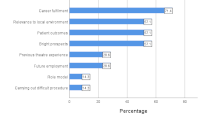
Results: Fifty-five of 85 (64.7%) residents responded. The majority were male (81.8%) with a mean age of 33 ± 3.5 years. Only 7 (12.7%) residents planned to pursue paediatric surgery. No statistically significant association was found between the intention to specialize and prior exposure to paediatric surgery (p = 0.269) or having a role model in the field (p = 0.869). Common deterrents included unfriendly trainers (8; 16.7%), the demanding nature of the specialty (6; 12.5%), and challenges with paediatric procedures such as intravenous access (6; 12.5%). Conversely, those who planned to specialize cited career fulfillment (5; 71.4%), relevance to local needs (4; 57.1%), and perceived good outcomes (4; 57.1%) as key motivators.
Conclusion: Despite exposure and mentorship, few junior residents intend to specialize in paediatric surgery. The attitude of trainers and perceived clinical challenges may discourage interest while personal fulfillment and contextual relevance could inspire commitment. Addressing interpersonal and systemic barriers may help strengthen the paediatric surgery workforce in Nigeria.
References
United Nations. Transforming our world: the 2030 Agenda for Sustainable Development. 2015.
Woods A, Shofner C, Hodge B. International pediatric surgery partnerships in sub-Saharan Africa: a scoping literature review. Glob Health Action. 2022; 15(1): 2111780
https://doi.org/10.1080/16549716.2022.2111780
Bickler SW, Rode H. Surgical services for children in developing countries. Bull World Health Organ. 2002; 80(10): 829 – 835
Meara JG, Leather AJM, Hagander L, et al. Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet. 2015; 386(9993): 569 – 624
Ozgediz D, Poenaru D. The burden of pediatric surgical conditions in low and middle-income countries: a call to action. J Pediatr Surg. 2012; 47(12): 2305 – 2311.
Krishnaswami S, Nwomeh BC, Ameh EA. The pediatric surgery workforce in low-and middle-income countries: problems and priorities. Semin Pediatr Surg. 2016; 25(1): 32 – 42 https://doi.org/101053/j.sempedsurg.2015.09.007
Inglin S, Bara A. Development of sustainable global pediatric surgery: Pioneering solutions from Burkina Faso. World J Surg. 2025; 49(3): 695 – 697
https://doi.org/10.1002/wjs.12430
Tyson AF, Msiska N, Kiser M, Samuel JC, McLean S, Varela C, et al. Delivery of operative pediatric surgical care by physicians and non-physician clinicians in Malawi. Int J Surg. 2014; 12(5): 509 – 515. https://doi.org/10.1016/j.ijsu.2014.02.009
Zafar SN, McQueen KA. Surgery, public health, and Pakistan. World J Surg. 2011; 35(12): 2625 – 2634
Schwartz MD, Durning S, Linzer M, et al. Changes in medical students’ views of internal medicine careers from 1990 to 2007. Arch Intern Med. 2011; 171(8): 744 – 749
Buddeberg-Fisher B, Klaghofer R, Abel T, et al. Swiss residents’ specialty choices – impact of gender, personality traits, career motivation and life goals. BMC Health Serv Res. 2006; 6: 137
Ekenze SO, Ajuzieogu OV, Nwomwh BC. Paediatric Surgery in Africa: how close are we to meeting the needs? World J Surg. 2011; 35(1): 17 – 22
Glynn RW, Kerin MJ. Factors influencing medical students and junior doctors in choosing a career in surgery. The Surgeon. 2010; 8(4): 187 – 191
https://doi.org/10.1016/j.surge.2009.11.005
Falase B, Olufemi S, Adeleye A, Amogbonjaye A, Sunmola S, Olaiya A, et al. Career choices and determining factors among final year medical students in Lagos, Nigeria. Nig J Med. 2022; 31(4): 390 – 395. https://doi.org/10.4103/NJM.NJM_38_22
Compton MT, Frank E, Elon L, Carrera J. Changes in U.S. medical students’ specialty interests over the course of medical school. J Gen Intern Med. 2008; 23(7): 1095 – 1100
https://doi.org/10.1007/s11606-008-0579-z
Sinclair P, Fitzgerald JEF, McDermott FD, Derbyshire L, Shalhoub J. Mentoring during surgical training: Consensus recommendations for mentoring programmes from the Association of Surgeons in Training. Int J Surg. 2014; 12(3): 55 – 58
https://doi.org/10.1016./ijsu.2014.08.395
Olajide T, Ezebialu C, Uche-Orji C, Abdullateef R, Okoye C, Olaoye E, et al. Specialty preferences among Nigerian medical students: a cross-sectional study. 2025; 25(628)
https://doi.org/10.1186/s12909-025-07189-5
Peel JK, Schlachta CM, Alkhamesi NA. A systematic review of the factors affecting the choice of surgery as a career. Can J Surg. 2018; 61(1): 58 – 67. https://doi.org/10.1503/cjs.008217
Holmer H, Bekele A, Hagander L, Harrison EM, Kamali P, Ng-Kamstra JS et al. Evaluating the collection, comparability and findings of six global surgery indicators. Br J Surg. 2019; 106(2): 138 – 150 https://doi.org/10.1002/bjs.11061