High-Risk Cervical Human Papillomavirus Prevalence in a Northeast Nigeria Community: A Descriptive Study
Main Article Content
Keywords
Cervical cancer screening, Human papillomavirus, Pap Smear, Northeast Nigeria, Genotype
Abstract
Background: Disparities in cervical screening result in disproportionate cervical cancer burdens in populations. This study assessed cervical human papillomavirus (HPV) infection prevalence in a rural northeast Nigeria community with low access to cervical screening.
Methodology: A community health outreach was conducted at a primary healthcare facility in Azare, Bauchi State, Nigeria. The women who wished to and consented to undergo gynaecological consultations were non-randomly enrolled on the study and provided their sociodemographic data and cervical specimens (Pap smear and cytobrush exfoliates in viral transport media) for the study. These were analysed cytologically and for the presence of HPV deoxyribonucleic acid (DNA).
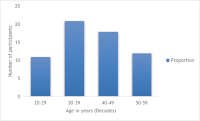
Results: Of 62 women screened (mean age 38.5 ± 9.8 years), 34 (54.8%) tested positive for HPV DNA (95% confidence interval = 43-67%). Among these positive cases, 19 had no intraepithelial lesion or malignancy (NILM), 8 were designated atypical squamous cell of undetermined significance (ASCUS), and 6 showed low-grade squamous intraepithelial lesion (LSIL). In contrast, one case was high-grade SIL (HSIL). Thirty single infections were seen, HPV 16 being the commonest (18 cases), followed by HPV 18 (9 cases), while non-16, non-18 genotypes (genotypes 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 66, 67, 68), collectively termed “Others”, accounted for 3 cases. Coinfections among different genotype classes (genotypes 16, 18 and Others) occurred in 4 additional cases. Most of the women had a primary education or higher (43; 69.4%), were married (53; 85.5%), and were multiparous (52; 83.9%). However, the majority had not heard about cervical cancer (35; 56.5%), while 60 (96.8%) women had never been screened previously.
Conclusions: The results suggest a high prevalence of cervical HR-HPV and SIL in Azare. Improved public enlightenment and access to cervical cancer screening services may help to decrease transmission of HPV and subsequent cervical cancer in the population.
References
2. Okunade KS. Human papillomavirus and cervical cancer. Journal of Obstetrics and Gynaecology [Internet] 2020 [cited 2025 Nov 21];40(5):602–8. Available from: https://www.tandfonline.com/doi/full/10.1080/01443615.2019.1634030
3. Emeribe AU, Abdullahi IN, Etukudo MH, Isong K, Emeribe AO, Nwofe JO, et al. The pattern of human papillomavirus infection and genotypes among Nigerian women from 1999 to 2019: a systematic review.
4. Manga MM, Fowotade A, Abdullahi YM, El-nafaty AU, Adamu DB, Pindiga HU, et al. Epidemiological patterns of cervical human papillomavirus infection among women presenting for cervical cancer screening in North-Eastern Nigeria. Infect Agents Cancer [Internet] 2015 [cited 2024 June 22];10(1):39. Available from: http://www.infectagentscancer.com/content/10/1/39
5. Okoeguale J, Samuel SO, Amadi SC, Njoku A, Okome GBO. Prevalence and distribution of cervical high-risk human papillomavirus infection in a rural community of Edo State, Nigeria: Prévalence et répartition de l’infection cervicale à haut risque par le virus du papillome humain dans une communauté rurale de l’État d’Edo, au Nigér. Af J Clin Exp Micro [Internet] 2022 [cited 2025 Nov 21];23(4):437–41. Available from: https://www.ajol.info/index.php/ajcem/article/view/234657
6. Dom-Chima N, Ajang YA, Dom-Chima CI, Biswas-Fiss E, Aminu M, Biswas SB. Human papillomavirus spectrum of HPV-infected women in Nigeria: an analysis by next-generation sequencing and type-specific PCR. Virol J [Internet] 2023 [cited 2025 Nov 21];20(1):144. Available from: https://virologyj.biomedcentral.com/articles/10.1186/s12985-023-02106-y
7. Ogundipe L, Ojo T, Oluwadare T, Olayemi E, Oluwafemi F, Oni O, et al. Cervical cancer screening and vaccination: knowledge, awareness, and attitude of female staff in a Nigerian University. BMC Women’s Health [Internet] 2023 [cited 2025 Nov 22];23(1):218. Available from: https://bmcwomenshealth.biomedcentral.com/articles/10.1186/s12905-023-02345-9
8. Okunowo AA, Anumni CC, Habeebu MY, Olayioye OM. Reproductive and Sexual Predictors of Late-Stage Cervical Cancer Presentation in Lagos, Nigeria. Cureus [Internet] 2025 [cited 2025 Oct 5];Available from: https://www.cureus.com/articles/354281-reproductive-and-sexual-predictors-of-late-stage-cervical-cancer-presentation-in-lagos-nigeria
9. Schnatz PF, Markelova NV, Holmes D, Mandavilli SR, O’Sullivan DM. The Prevalence of Cervical HPV and Cytological Abnormalities in Association with Reproductive Factors of Rural Nigerian Women. Journal of Women’s Health [Internet] 2008 [cited 2025 Oct 5];17(2):279–85. Available from: http://www.liebertpub.com/doi/10.1089/jwh.2006.0295
10. Schluterman NH, Sow SO, Traore CB, Bakarou K, Dembelé R, Sacko F, et al. Differences in patterns of high-risk human papillomavirus infection between urban and rural low-resource settings: cross-sectional findings from Mali. BMC Women’s Health [Internet] 2013 [cited 2025 Nov 21];13(1):4. Available from: https://bmcwomenshealth.biomedcentral.com/articles/10.1186/1472-6874-13-4
11. Runge I, Klein JMA, Pannen AK, Abera S, Wakuma T, Gebrehiwot Y, et al. Prevalence of human papillomaviruses in self-collected samples among women attending antenatal care in Ethiopia: a cross-sectional study.
12. Shahramian I, Heidari Z, Mahmoudzadeh-Sagheb H, Moradi A, Forghani F. Prevalence of HPV Infection and High Risk HPV Genotypes (16, 18), among Monogamous and Polygamous Women, In Zabol, Iran. 2011;40.
13. Nejo YT, Olaleye DO, Odaibo GN. Prevalence and Risk Factors for Genital Human Papillomavirus Infections Among Women in Southwest Nigeria. 2018;
14. Sauvaget C, Nene BM, Jayant K, Kelkar R, Malvi SG, Shastri SS, et al. Prevalence and Determinants of High-Risk Human Papillomavirus Infection in Middle-Aged Indian Women. Sexually Transmitted Diseases [Internet] 2011 [cited 2025 Oct 20];38(10):902–6. Available from: https://journals.lww.com/00007435-201110000-00004
15. J Mafiana J, Dhital S, Halabia M, Wang X. Barriers to uptake of cervical cancer screening among women in Nigeria: a systematic review. Afr H Sci [Internet] 2022 [cited 2024 Oct 27];22(2):295–309. Available from: https://www.ajol.info/index.php/ahs/article/view/228970
16. Agorastos T, Chatzistamatiou K, Katsamagkas T, Koliopoulos G, Daponte A, Constantinidis T, et al. Primary Screening for Cervical Cancer Based on High-Risk Human Papillomavirus (HPV) Detection and HPV 16 and HPV 18 Genotyping, in Comparison to Cytology. PLoS ONE [Internet] 2015 [cited 2025 Nov 22];10(3):e0119755. Available from: https://dx.plos.org/10.1371/journal.pone.0119755
17. Schiffman M, De Sanjose S. False positive cervical HPV screening test results. Papillomavirus Research [Internet] 2019 [cited 2025 Nov 22];7:184–7. Available from: https://linkinghub.elsevier.com/retrieve/pii/S2405852118301423
18. Bessa Y, Moore A, Eldemire F. Knowledge of Risk Factors for Cervical Cancer among Women in Togo. JSSW [Internet] 2017 [cited 2025 Nov 21];5(2). Available from: http://jsswnet.com/vol-5-no-2-december-2017-abstract-1-jssw
19. Li H, Xiao Z, Xing B, Wu S, Wang Y, Liu Z, et al. Association between common vaginal and HPV infections and results of cytology test in the Zhoupu District, Shanghai City, China, from 2014 to 2019. Virol J [Internet] 2022 [cited 2025 Nov 22];19(1):127. Available from: https://virologyj.biomedcentral.com/articles/10.1186/s12985-022-01850-x
20. Zhao F hui, Forman MR, Belinson J, Shen Y hong, Graubard BI, Patel AC, et al. Risk factors for HPV infection and cervical cancer among unscreened women in a high-risk rural area of China. Int J Cancer [Internet] 2006 [cited 2025 Oct 20];118(2):442–8. Available from: https://onlinelibrary.wiley.com/doi/10.1002/ijc.21327